Cornea and Refractive
What is Cornea and Refractive Surgery?
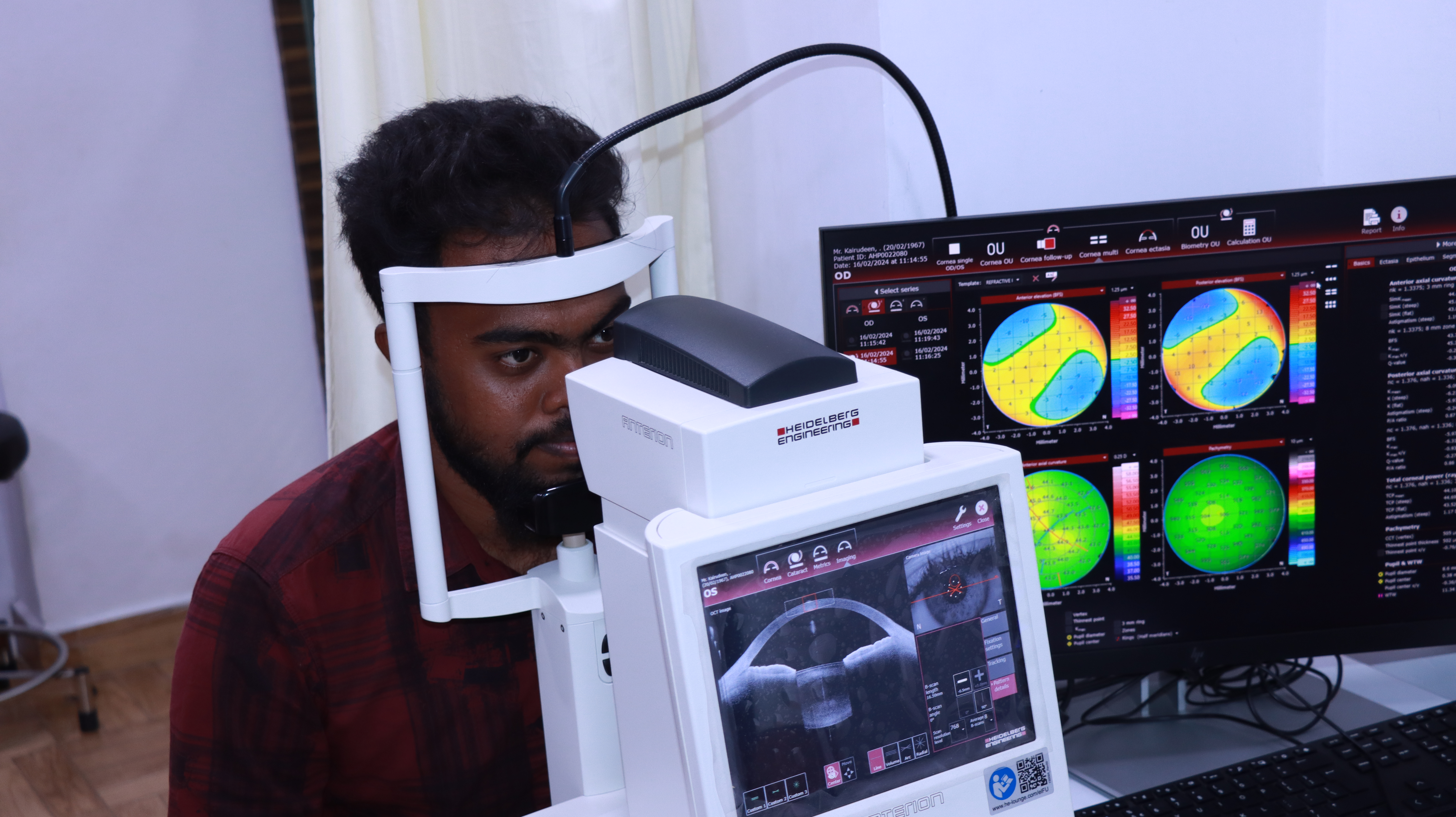
The Cornea is the transparent part of the eye where the vision correction surgery is carried out. Recent years have seen huge advances in this field. Refractive and laser eye surgery allow patients to see better than at any other time in their lives. Most of the time patients may give up using eyeglasses or contact lenses altogether after this surgery.
Types Of Refractive Surgeries
LASIK, EPI LASIK, FEMTO LASIK, and SMILE LASIK are vision correction surgeries that mainly reshape the cornea in the eye i.e. the clear front part of your eye which allows light to travel through it and focus properly on the back of your eye the retina.
Whereas ICL is not performed on the cornea, it is an intracollamer contact lens fixed permanently inside the eye to correct the refractive power of the eye that is still considered as refractive surgery because corrects the refractive power of the eye.
Refractive surgery is a procedure to correct the refractive error and make him/her spectacle free. There are basically 3 types of refractive surgery.
1. Corneal laser procedure called LASIK surgery spherical power upto +6.00 to -8. 00 Diopter can be corrected and cylindrical.
Microkeratome blade LASIK power upto 4 Diopter can be correct with this procedure
EPILASIK is a surface procedure where we ablate the cornea after removing the superficial epithelium. This is done in thin cornea and has a relatively longer healing time.
FEMTO BLADE FREE LASIK in a more advanced and more presice surgery where a thinner flap can be made with a femtosecond laser machine.
SMILE LASIK is the latest advancement in refractive surgery where a thin lenticule is removed from the corneal stroma through a 2mm incision. This avoids the step of flap creation .
2. ICL (IMPLANTABLE CONTACT LENS) is a procedure for high powers that cannot be frected with LASIK. Cylindrical power can be also corrected with toric ICL. This contact lens is placed between the iris & the natural lens. This is also permanent procedure.
3. RLE ( Refractive lens exchange) is similar to cataract surgery but before the cataract forms. This is preferred for people who are more than 40 years old & do not want glasses for reading. Multifocal lens can be implanted for them. They will not require cataract surgery in future. The natural lens is replaced by an artificial lens of the required power.
TYPES OF CORNEAL SURGERIES
Corneal surgery is replace of corneal part with corneal tissue from a donor like PKP,TKP. Whereas, C3R is done for the Keratoconus condition.
Advantages of LASIK Surgery
- After LASIK, patients no longer require vision glasses or contact eyes
- LASIK can completely change the vision condition and correct the lost sight
- Painless since numbing eye drops are used
- Vision gets corrected almost immediately or the next day after LASIK
- No bandages or stitches are required in this treatment
- Adjustments can be made years after LASIK in case further correction of vision is required in old age
At An-Noor Eye Hospital we also use Femto LASIK which is considered the most highly advanced technology. The inclusion of Femto Lasik in refractive error surgery has raised safety to a new level because the side effects and the tensions in the cornea are kept to a minimum. Also, this is an outpatient procedure and does not require hospitalization. Generally, anesthetic eye drops are used and the patient is awake during the entire procedure. Almost normal sight capacity is restored and the patient can enjoy the results the very same day following the surgery.
Benefits of Femto-Lasik are:
- Precise, safer and accurate procedure
- Painless, bladeless technique
- Very fast recovery period
- No complications as cuts are avoided
- Wider band of refractive error correction
- Patients ineligible for Lasik can use FEMTO LASIK

Our Testimonials
In the hospital were too nice to patients! ”

About Annoor Eye Hospital
An-Noor Eye Hospital is a NABH-accredited specialty eye hospital with the objective of making eye care available, accessible, and affordable to all strata of society.

Number of Patients Seen
Number of Surgeries Done
Total Camps
Patients Treated in Camps
Why Patients Choose Annoor Eye Hospital
We provide quality eye care by quality service at affordable cost. An Noor Eye Hospital is chosen for many reasons:
01
Advanced Equipments
“Along with all amenities, we have the best eye doctors at our
hospital”
The Experts &
02
Video Consultation
“Online Consultation to be received from the best eye Hospital in Chennai”
Home Visits &
03
NABH &
International Standard
“We follow international Standards
as per NABH for treatments and
clinical Examination”
04
03
Vision Therapy
“Along with all amenities, we have the best eye doctors & Clinical team at our
hospital”
05
04
EMI & Insurance
“We have medical insurance tie-ups with reputed health insurance companies making us a patient-friendly”
05
NABH & International Standard
“We follow international Standards
as per NABH for treatments and
clinical administration”